Unrecognised oesophageal intubation
Unrecognised oesophageal intubation has devastating consequences for all involved [1].
We summarise a case where unrecognised oesophageal intubation resulted in death from
hypoxic brain injury [2], and consider how human factors and ergonomics (HFE) strategies
might prevent harm from oesophageal intubation in the future.
Case summary
Glenda Logsdail, a fit and well 61 year old retired radiographer,
was anaesthetised for an emergency laparoscopic
appendicectomy in August 2020. Following pre-oxygenation
and induction of anaesthesia, a theatre practitioner attempted
intubation under the supervision of a consultant anaesthetist but
was unsuccessful. The consultant then proceeded to intubate,
but unfortunately placed the tracheal tube in the oesophagus
and failed to recognise this. Three minutes later she became
profoundly hypoxic; the anaesthetist misinterpreted the clinical
picture as anaphylaxis and treated accordingly. A prolonged
period of hypoxia culminated in cardiac arrest, a cardiac arrest call
was made and a second consultant anaesthetist attended. Eleven
minutes after the cardiac arrest call, the oesophageal intubation
was recognised and the tracheal tube placed correctly. Return
of spontaneous circulation occurred shortly after and she was
transferred to ICU. Unfortunately, the unrecognised oesophageal
intubation and subsequent prolonged hypoxia led to irreversible
brain injury and she died five days later. Of note, she did not have
a difficult airway, a standard Macintosh laryngoscope was used for
all intubations, and continuous waveform capnography was in use
throughout.
The Coroner issued a Regulation 28 ’Report to Prevent
Future Deaths’ and the RCoA, DAS, SALG and Association of
Anaesthetists are responding to this in detail. Glenda’s case
involves technical skill issues including accidental oesophageal
intubation and its delayed recognition, with minimal confirmatory
checks of tracheal intubation evident. In addition, the Coroner
commented on issues with non-technical skills: loss of situation
awareness and erroneous fixation on the anaphylaxis diagnosis;
team malfunction with “chaos and panic” in the anaesthetic room
and confusion regarding roles; absence of a leader, with the
lead anaesthetist “effectively blind to what needed to be done”;
an “inhibitory team hierarchy” preventing other team members
speaking out; and lack of standardisation of anaesthetic machine
and ventilator monitors [2].
Human factors and ergonomics
HFE is a scientific discipline that ‘makes it easy to do the right thing
and difficult, or ideally impossible, to do the wrong thing’ [3]. Its
underlying principles are that, as humans, we are liable to make
mistakes and that relying on personal performance – common in
healthcare – is not a failsafe method of ensuring patient safety.
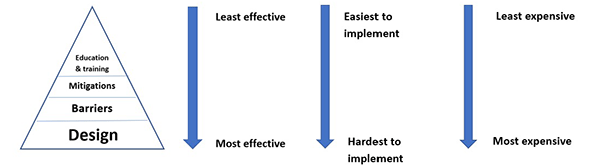
HFE strategies can be described using the ‘hierarchy of controls’
model (Figure 1) [4], with strategies arranged as a pyramid in
order of likely effectiveness.
Design
Design of safe systems, including equipment and working
environment, is most likely to be effective and aims to prevent
error occurring. Such design strategies are used in all UK safety-critical
industries and account for ≈90% of safety improvements.
Equipment design to prevent harm from oesophageal intubation
includes videolaryngoscopy to increase first-pass intubation rate
and reduce failed intubation, especially in patients with difficult
airways [5]. Videolaryngoscopy offers communication benefits,
with all team members able to see the view at laryngoscopy
(‘changing intubation from me to we’), allowing the anaesthetic
assistant to apply or adjust cricoid pressure, anticipate the next
step and call for help if needed. These features flatten the team
hierarchy and improve the recognition of oesophageal intubation.
Videolaryngoscopy also improves intubation training [5].
Monitor design was highlighted by the Coroner after one
anaesthetist mistook the airway pressure waveform for a
capnography trace. SALG and industry colleagues are therefore
discussing standardisation of the location and colour of the
capnography trace on anaesthetic machine monitors and
ventilators, and the use of ‘smart alarms’ that may improve
detection of oesophageal intubation [6].
Design of the working environment during laryngoscopy can be
optimised by positioning the videolaryngoscope screen on the
opposite side of the bed to the anaesthetic assistant, enabling all
team members to see the view at laryngoscopy, and improving
recognition of oesophageal intubation. The Coroner commented
on the cramped conditions in the anaesthetic room: induction
of anaesthesia in the operating theatre provides more space for
equipment and staff should an emergency occur.
Barriers
Barriers are HFE strategies that aim to ‘trap’ errors and prevent a
patient coming to harm after oesophageal intubation. Examples
include using capnography for all intubations, with the whole
multidisciplinary team trained to recognise capnography
waveforms and understand the significance of a flat trace [7].
In addition, a two-person verbal intubation check, with the
intubator and anaesthetic assistant both visualising the tracheal
tube passing through the vocal cords on the videolaryngoscope
screen and confirming the presence of a capnograph trace on
the monitor, has been proposed to improve the detection of
oesophageal intubation.
Barriers also include the use of non-technical skills [8] during
everyday work, including: use of team members’ first names; a
verbal pre-induction team safety brief during preoxygenation
confirming airway management plans; and specific tools
including closed loop communication, standardised handover
tools and graded assertiveness tools [8].
Mitigations
Mitigations are HFE strategies that reduce the consequences
of an error, providing a final attempt to reduce harm from
unrecognised oesophageal intubation. These include crisis
management tools, non-technical skills and tools for regaining
situation control in conditions of cognitive overload. Other
mitigations include peer support tools that may reduce the
impact of critical events on team members; these include Trauma
Risk Management (TRiM), developed by the UK Armed Forces
and recently introduced into healthcare [9].
Education, training, rehearsal and simulation
Education and training are essential for safety but will only be
effective if other HFE strategies are in place; if a well-trained
team is placed into an unsafe working environment then an error
is likely to occur [4]. Education and training to prevent harm from
unrecognised oesophageal intubation should include simulation
training, including non-technical and crisis management skills,
and out-of-theatre airway workshops covering airway rescue
techniques. Optimising technical skills, including the technique
required to use a hyperangulated videolaryngoscope blade, can
‘make room in one’s head’ for good non-technical skills. Training
should be regular to prevent ‘skill decay’, multidisciplinary to flatten the team hierarchy, and arguably mandatory. Protected
time should be allocated for staff to organise, run and attend
training.
In summary, NAP4 included nine cases of oesophageal
intubation, but 10 years after its publication patients are
still dying following unrecognised oesophageal intubation.
This might be prevented by: designing strategies to prevent
oesophageal intubation occurring in the first place, potentially
using videolaryngoscopes for all intubations; using methods
to detect oesophageal intubation rapidly when it occurs by
promoting capnography use and waveform recognition;
protected time for multidisciplinary regular airway workshop
and simulation training; and potentially making such training
mandatory.
Figure 1. 'Hierarchy of controls' model
Paula Joy
Specialist Registrar
Fiona E Kelly
Consultant
Department of Anaesthesia and Intensive Care Medicine
Royal United Hospitals Bath NHS Foundation Trust, Bath
Twitter: @fionafionakel
References
- Cook TM, Harrop-Griffiths W. Capnography prevents avoidable deaths. British
Medical Journal
2019; 364: 1439.
- Judiciary.UK. In the Milton Keynes Coroner’s Court. Inquest into the death of
Glenda May Logsdail, Regulation 28: report to prevent future deaths, 2021.
https://www.judiciary.uk/wp-content/uploads/2021/09/Glenda-Logsdail-Prevention-of-future-deaths-report-2021-0295_Published.pdf (accessed
25/11/2021).
- Kelly FE, Bhagrath R, McNarry AF. The ‘airway spider’: an education tool to assist
teaching human factors and ergonomics in airway management.
Anaesthesia
2018; 73: 257-8.
- Liberati EG, Peerally MF, Dixon-Woods M. Learning from high risk industries
may not be straightforward: a qualitative study of the hierarchy of risk controls
approach in healthcare.
International Journal for Quality in Health Care 2018; 30:
39-43.
- Kelly FE, Cook TM. Seeing is believing: getting the best out of
videolaryngoscopy.
British Journal of Anaesthesia 2016; 117: i9-13.
- Pandit JJ, Young PJ, Davies M. Why does oesophageal intubation still go
unrecognised? Lessons for prevention from the coroner's court.
Anaesthesia
2021; in press.
- Royal College of Anaesthetists. Capnography: No trace = wrong place, 2021.
https://rcoa.ac.uk/safety-standards-quality/guidance-resources/capnography-no-trace-wrong-place (accessed 25/11/2021).
- Flin R, Patey R, Glavin R, Maran N. Anaesthetists’ non-technical skills. British
Journal of Anaesthesia
2010; 105: 38-44.
- Kelly FE, Osborn M, Stacey MS. Improving resilience in anaesthesia and intensive
care medicine – learning lessons from the military.
Anaesthesia 2020; 75: 720-3.